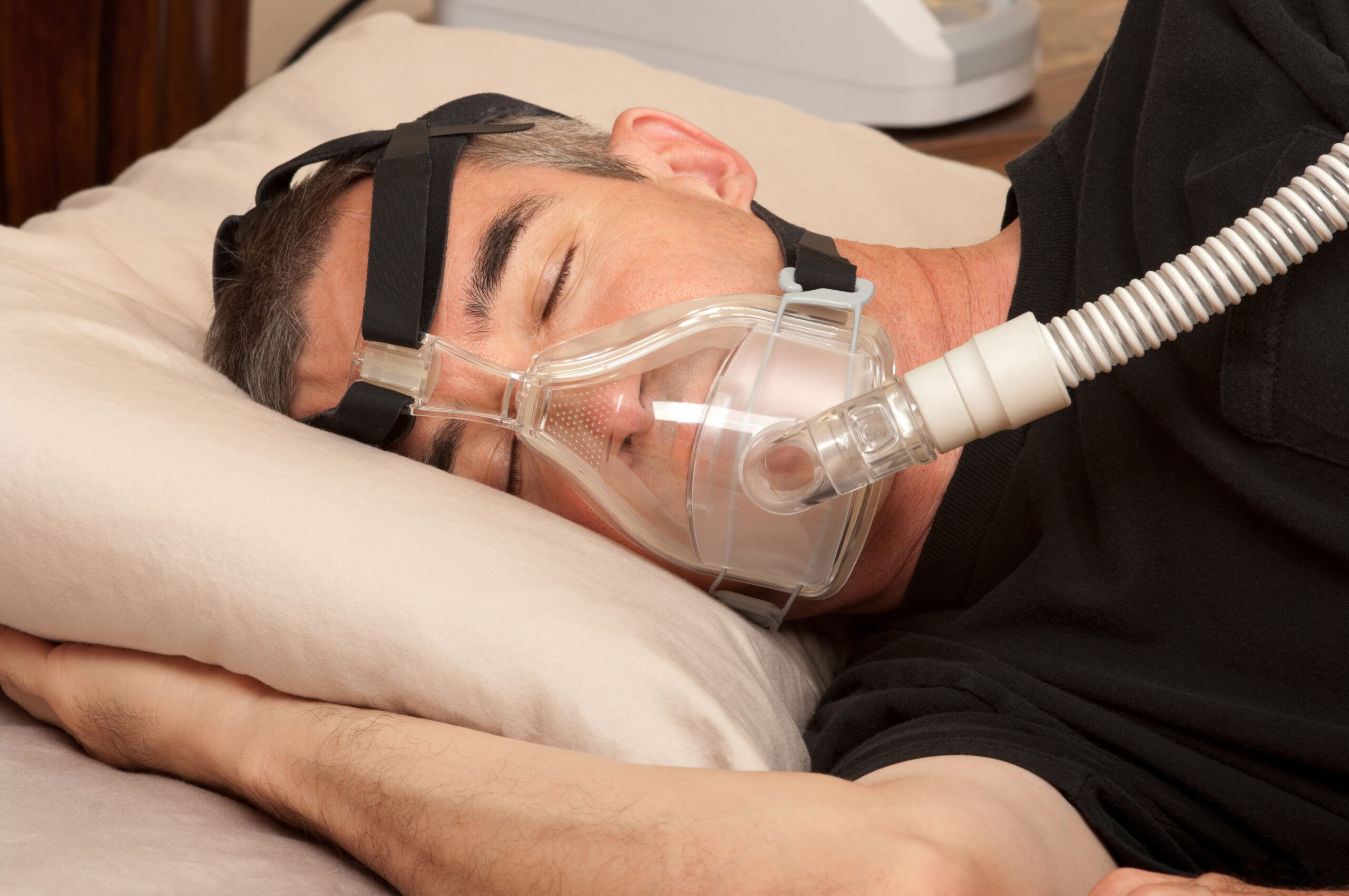
Sufferers of breathing disorders such as sleep apnea are usually thought to be at higher risk for cardiovascular disease. A new study from Technion-Israel Institute of Technology scientists suggests that some heart attack patients with these conditions may actually benefit from mild to moderate sleep-disordered breathing.
Apnea and other types of sleep-disordered breathing can boost the numbers and functions of rare cells that help to repair and build new blood vessels, according to the Technion’s Dr. Lena Lavie and her colleagues. They say the findings could help predict which patients are at a greater health risk after a heart attack, and may even suggest ways to rebuild damaged heart tissue.
Lavie, along with researchers Dr. Slava Berger, Prof. Doron Aronson and Prof. Peretz Lavie, studied 40 male patients—a mix of healthy sleepers and those with sleep disordered breathing—who had had a heart attack just a few days earlier.
Blood samples drawn from these patients revealed that the sleep disordered breathing patients had markedly higher levels of endothelial progenitor cells (EPCs), which give rise to new blood vessels and repair the injured heart, than the healthy sleepers. They also had higher levels of other growth-promoting proteins and immune cells that stimulate blood vessel production.
“Heart attack is a potent stimulus for EPC mobilization,” said Aronson. He also explained that the cells move from bone marrow to the heart to repair damaged tissue after a heart attack.
“The field of cell-based cardiac repair has struggled to find the best approach to enhance recruitment of EPCs to the heart following myocardial infarction,” said Aronson. The Technion findings, he said, suggest that intermittent periods of oxygen deprivation in heart attack patients “provides a simple and powerful means to boost EPC mobilization.”
“It should be further investigated if inducing intermittent hypoxia immediately after a heart attack, in patients without sleep disordered breathing, will also have such an effect,” Lavie said.
The study was published in the American Journal of Respiratory and Critical Care Medicine.
Fighting for Israel's truth
We cover what makes life in Israel so special — it's people. A non-profit organization, ISRAEL21c's team of journalists are committed to telling stories that humanize Israelis and show their positive impact on our world. You can bring these stories to life by making a donation of $6/month.