Treatment of breast cancer today tends to be standard, but as doctors know only too well, not all breast cancers are the same. Some are malignant, some are not.
Now, Israeli scientists have developed a new way of identifying malignant cancer cells at an earlier stage to help physicians create effective customized treatments for every individual patient, potentially saving thousands of lives.
Breast cancer is the second leading cause of cancer deaths in women in the US today, after lung cancer. One in eight US women will experience breast cancer sometime in their lives. Worldwide 1.3 million women are diagnosed with breast cancer annually, according to the American Cancer Society, and about 465,000 will die from the disease.
The problem with existing treatments is that many women do not receive the therapy that actually fits their disease. Some tumors will metastasize, some will not – up to now clinicians found it difficult to determine which tumor is which.
Identifying cancer metastasis before it spreads
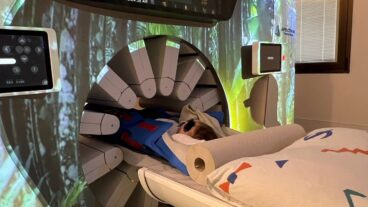
Using a combination of MRI and ultrasound imaging, researchers at Tel Aviv University (TAU) have discovered a way to measure the metabolic changes that occur during cancer metastasis. Increased blood flow (which can be sensed by ultrasound) and an increase of oxygen consumption (measured with an MRI) can indicate cancer metastasis with unprecedented levels of sensitivity.
Normally scientists look for structural changes in the body, such as the presence of a tumor. But using this method, the researchers led by Dr. Ilan Tsarfaty, from TAU’s Faculty of Medicine, are actually able to “see” cancer metastasis within a small group of cells long before the cancer spreads to other organs in the body.
This approach, which is supported by the Breast Cancer Research Foundation of America, helps determine, at an earlier stage than ever before, which cells are metastasizing, and how they should be treated. It will be tested in clinical trials beginning in 2010,
“We have developed a non-intrusive way of studying the metabolism of breast cancer in real time,” says Tsarfaty, whose wife – a radiologist – is part of his research team. “It’s an invaluable tool. By the time results are in from a traditional biopsy, the cancer can already be radically different. But using our technique, we can map the tumor and its borders and determine with high levels of certainty – right away – which patients should be treated aggressively.
Tailoring treatment to individual patients
“Current breast cancer treatments are not tailored to individual patients,” Tsarfaty adds. “Our approach to profiling individual tumors will not only help save lives today, it will provide the basic research for developing cancer drugs of the future,” he says.
The research, which is now taking place at Israeli hospitals, falls in a new field called “translational and personalized medicine”. Papers describing Tsarfaty’s work were published recently in the journals Cancer Research and Neoplasia.
The new research can be applied to all solid tumors, including those resulting from lung and brain cancer, and could also be used to respond to a wide spectrum of neurodegenerative diseases, such as Alzheimer’s, Tsarfaty reports.
“Today, clinicians only diagnose cancer when they see a tumor several millimeters in size. But our diagnosis can be derived from observing only a few cells, and looks specifically at the activation levels of a protein called Met. Activated Met is an oncogen,” says Tsarfaty, who is now working to establish a Molecular Imaging Center with a multi-disciplined approach to cancer imaging and treatment. “If the tumor cells show activation of Met, we can design personalized medicine to treat a specific kind of breast cancer.”