Antibiotic resistant bacteria and antimicrobial-resistant fungi cause more than 2.8 million infections a year in the United States, resulting in some 35,000 deaths.
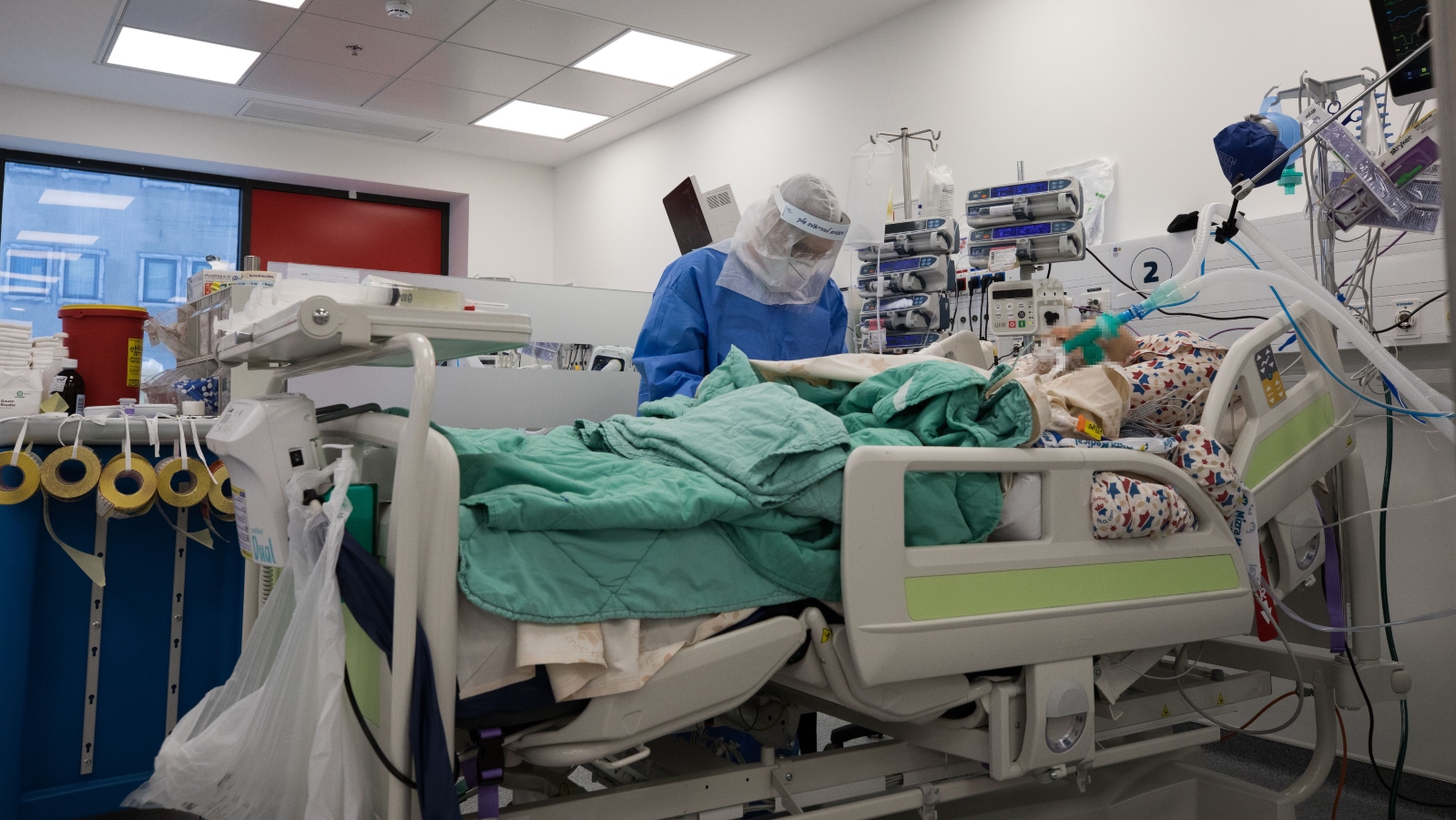
Moreover, these “superbugs” may be responsible for some Covid-19 deaths. One in seven people hospitalized with the Covid-19 virus has acquired a secondary bacterial infection. Half of the Covid-19 patients who have died had such infections, according to Julie Gerberding of pharmaceutical giant Merck, and a former head of the US Centers for Disease Control.
“The challenge of antibiotic resistance could become an enormous force of additional sickness and death across our health system as the toll of coronavirus pneumonia stretches critical care units beyond their capacity,” Gerberding predicted in Stat News earlier this year.
That’s what makes Hebrew University’s development of a solution for antibiotic-resistant bacteria so important.
The treatment is a repurposed topical antibiotic called mupirocin, been beefed up via nanotechnology so that it can be injected intravenously.
The team that created the new treatment was led by Prof. Yechezkel Barenholz, who heads the Laboratory of Membrane and Liposome Research at Hebrew University Hadassah Medical School, and Dr. Ahuva Cern, in collaboration with Prof. Amiram Goldblum. All three hail from the Hebrew University Faculty of Medicine.
Barenholz played a key role in developing Doxil, a chemotherapy drug based on nano-delivery.
Nano-mupirocin has been tested on animals and will now begin human trials on its way toward hoped-for FDA and European CE approval.
“This drug, if approved, fundamentally enhances the arsenal of antibiotics available to treat resistant infections, including those associated with Covid-19,” said Cern.
According to the European Antibiotic Resistance Organization, 700,000 people around the world die every year from antibiotic-resistant infections. If no significant improvement is made in the field, that number could rise to 10 million by 2050.
The Israeli research was supported by a grant from the National Institutes of Health and resulted from a study the Hebrew University researchers conducted with colleagues at the Helmholtz Centre for Infection Research in Germany.