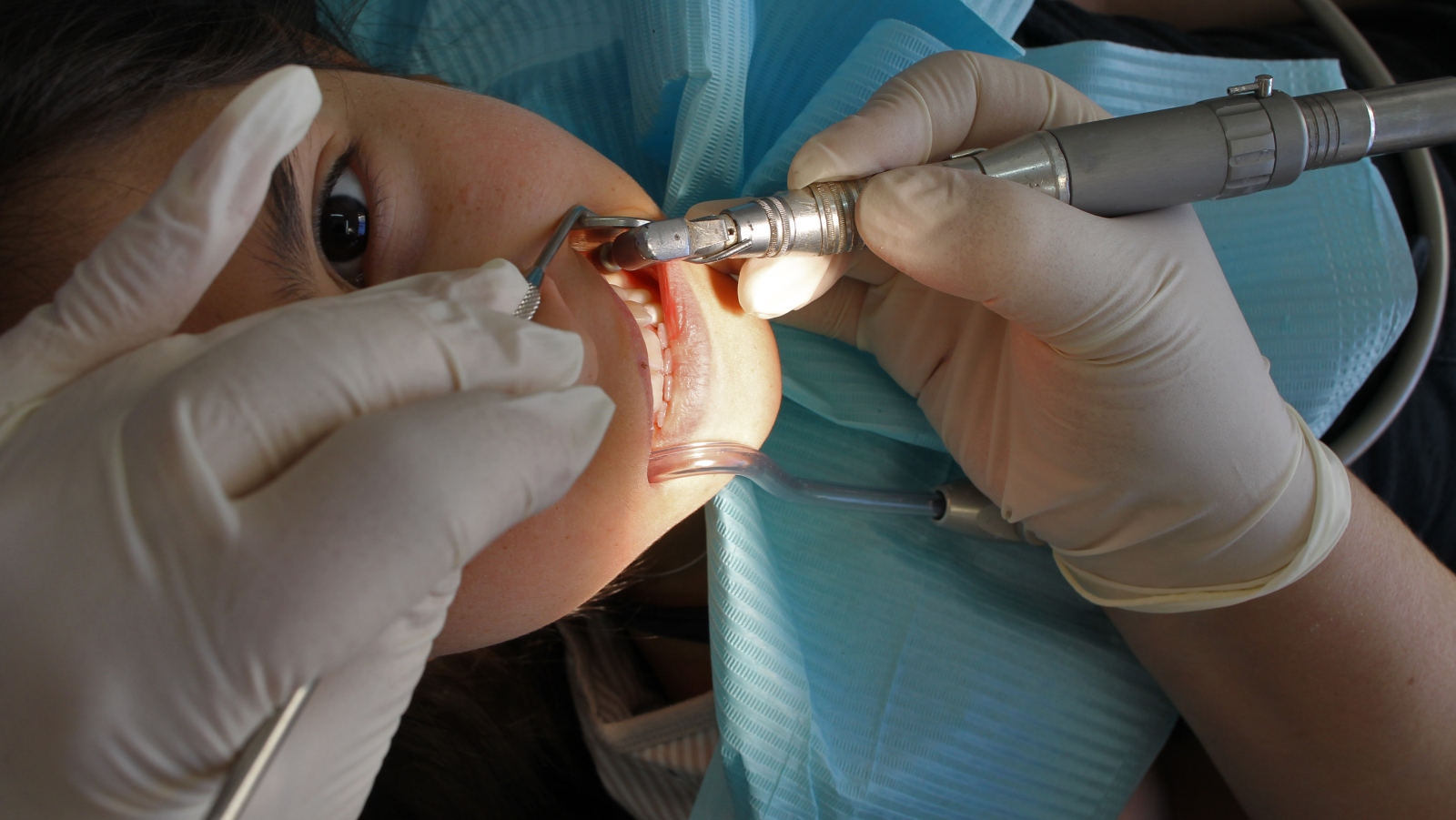
Novel dental fillings made of resin-based composites enhanced by antibacterial nano-assemblies, developed at Tel Aviv University, can hinder bacterial growth on dental restorations, the main cause of recurrent cavities that can lead to root-canal treatment and tooth extractions.
“Antibiotic resistance is now one of the most pressing healthcare problems facing society, and the development of novel antimicrobial therapeutics and biomedical materials represents an urgent unmet need,” said lead researcher Dr. Lihi Adler-Abramovich.

“When bacteria accumulate on the tooth surface, they ultimately dissolve the hard tissues of the teeth. Recurrent cavities — also known as secondary tooth decay — at the margins of dental restorations results from acid production by cavity-causing bacteria that reside in the restoration-tooth interface.”
She explained that the enhanced material is superior both to composite resins, which look good but don’t have any antibacterial effect, and antibacterial amalgam fillings composed of metal alloys that have problems of toxicity and lack of adherence.
The new material “is not only aesthetically pleasing and mechanically rigid but is also intrinsically antibacterial due to the incorporation of antibacterial nano-assemblies,” said TAU doctoral student Lee Schnaider.
The Israeli researchers were the first to discover the bacterial activity of the self-assembling building block Fmoc-pentafluoro-L-phenylalanine and devised a method of incorporating the nano-assemblies within dental composite restoratives.
“The minimal nature of the antibacterial building block, along with its high purity, low cost, ease of embedment within resin-based materials and biocompatibility, allows for the easy scale-up of this approach towards the development of clinically available enhanced antibacterial resin composite restoratives,” Adler-Abramovich said.
The researchers are evaluating the antibacterial capabilities of additional minimal self-assembling building blocks and developing methods to incorporate them into biomedical materials such as wound dressings and tissue scaffolds.
Other participants in the study, published recently in ACS Applied Materials and Interfaces, were Prof. Ehud Gazit, Prof. Rafi Pilo, Prof. Tamar Brosh, Dr. Rachel Sarig and colleagues from TAU’s Maurice and Gabriela Goldschleger School of Dental Medicine and George S. Wise Faculty of Life Sciences.