No egg, no sperm, no womb – researchers at Israel’s Weizmann Institute of Science grew synthetic embryo models of mice from stem cells cultured in a petri dish.
This model could help scientists study how stem cells form various organs in the developing embryo, and may one day make it possible to grow tissues and organs for transplantation using synthetic embryo models.
“The embryo is the best organ-making machine and the best 3D bioprinter. We tried to emulate what it does,” said Prof. Jacob Hanna of Weizmann’s Molecular Genetics Department, who headed the research team.
“Until now, in most studies, the specialized cells were often either hard to produce or aberrant, and they tended to form a mishmash instead of well-structured tissue suitable for transplantation. We managed to overcome these hurdles by unleashing the self-organization potential encoded in the stem cells.”

As described in the study published in Cell, Hanna’s team used two previous advances in his lab: an efficient method for reprogramming stem cells back to their earliest stage and an electronically controlled device for growing natural mouse embryos outside the womb.
In the current experiment, 50 of around 10,000 stem cells successfully developed into embryo-like structures. By eight and a half days later — nearly half of the mouse 20-day gestation – each embryo had formed a beating heart, blood stem cell circulation, a brain with well-shaped folds, a neural tube and an intestinal tract.
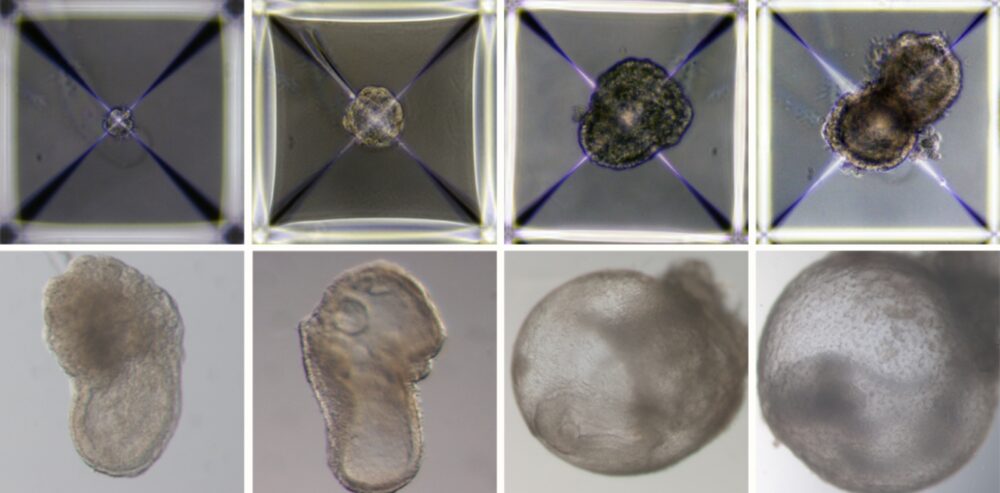
Compared to natural mouse embryos, the synthetic models displayed a 95 percent similarity in the shape of internal structures and the gene expression patterns of different cell types.
Growing a synthetic embryo model solely from stem cells cultured in a petri dish could, to a large extent, help researchers avoid the technical and ethical issues involved in using human embryos in research and biotechnology.
Even with mice, certain experiments are currently impossible because they would require thousands of embryos. The stem-cell embryos could be grown in incubators by the millions.
“Our next challenge is to understand how stem cells know what to do – how they self-assemble into organs and find their way to their assigned spots inside an embryo,” said Hanna.
“And because our system, unlike a womb, is transparent, it may prove useful for modeling birth and implantation defects of human embryos.”
In addition to helping reduce the use of animals in research, synthetic embryo models might in the future become a reliable source of cells, tissues and organs for transplantation.
“Instead of developing a different protocol for growing each cell type – for example, those of the kidney or liver – we may one day be able to create a synthetic embryo-like model and then isolate the cells we need. We won’t need to dictate to the emerging organs how they must develop. The embryo itself does this best,” Hanna said.