The African country will implement the Terem clinics’ remote consultation technologies to treat patients who don’t require a hospital visit.
The Kenyan Health Ministry has decided to adopt the Jerusalem-based model of Terem independent emergency medical centers and set up a similar chain of clinics of its own, a move that will likely transform the African country’s health-care system.
“The Kenyans are very dynamic people who are trying really hard to have a successful, democratic, prosperous society,” says Terem’s assistant medical director Dr. Nahum Kovalski.
Earlier this year, the Kenyan Health Ministry’s director-general came to Jerusalem to see the clinics in action. “They want to set up close to 50 community-based emergency care clinics, each servicing a few hundred thousand people in surrounding communities,” Kovalski tells ISRAEL21c.
“This is a huge project — reshaping a health system for a country of 35 million people.”
Terem operates five urgent care centers in the Jerusalem area, with more than 250,000 patient visits a year. Only seven percent of them get referred to hospitals. Israeli Health Ministry statistics show that per capita, 30 to 50 percent fewer patients turn up at hospital ERs in areas also served by Terem, meaning that the system significantly reduces stress on emergency rooms.
“A simple ankle fracture doesn’t need to go through a hospital. We X-ray the injury, then treat it,” he says. “Most fractures can be cast on the spot. Then we send them home. The patient pays a maximum of NIS 86 [about $22].” The primary care physician provides follow-up care.
Real-time remote consultations
What particularly interested the Kenyans, says Kovalski, is Terem’s use of the latest medical and communication technologies.
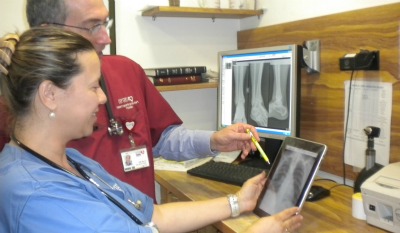
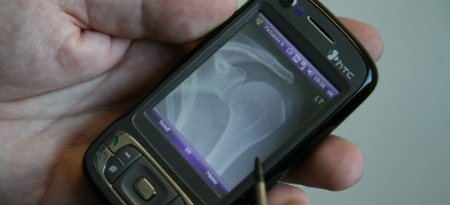
“Access to remote consultation tools is key. We have the ability in real time to review material together. Say a doctor wants a second opinion on an X-ray: It can be sent anywhere, via mobile phone or computer interface. We were one of the first groups in the world to use consultations via mobile phones in a real-time environment.”
Inaugurated in 1989, Terem was the brainchild of Dr. David Appelbaum, a Detroit-born rabbi and specialist in internal and emergency medicine, who was tragically killed in a 2003 terrorist bombing in Jerusalem. Today the company employs more than 200 people.
Kovalski, who headed teams of Terem physicians on study tours of Kenya, earned a computer science degree at McGill University in Canada before studying medicine.
“You have to communicate with local doctors and custom-design each system for its market,” he says, noting that most households in Kenya have mobile phones and Internet speed there is improving.
“We are doctors who understand technology, not just technologists who understand medicine. We understand the medical needs and can customize the solutions.
“As long as you have Internet, you can have real-time streaming of information. By using portable ultrasound devices, we can revolutionize health care. We’re going to see a lot more use of ultrasound in the future — I’ve heard it said that ultrasound is the stethoscope of the 21st century.”
Proximity will save lives
Another major advantage of the planned clinics is their accessibility. Kovalski points out that the primary killers of children in the Third World are dehydration and pneumonia — “simple” diseases, he calls them. “If you can get medical care closer to communities, instead of having them walk another day to a hospital, it will save lives.” The clinics also will offer community health education.
“At this point we have a complete package. Oracle is providing the infrastructure, including computers, servers, Internet and software support.”
The Medical Consultancy and Construction Group (http://www.mccgrouplondon.com), which Kovalski says “builds field hospitals like Lego,” is responsible for linking the components.
“We’ll be doing the training, and will bring specialist teams to develop customized software for their problems,” he says. “We have a large number of well-trained, dynamic doctors who want to be part of this project.”
The World Bank is expected to provide funding for the project.
Kovalski is confident that this is the right time to enact changes in approaches to medical care.
“It’s almost a perfect storm. As cell phone technologies come of age, this combination of medical knowledge as a package is pretty unique. We’ve already been approached by other African countries. Once it’s working in Kenya, it’ll take off.”












